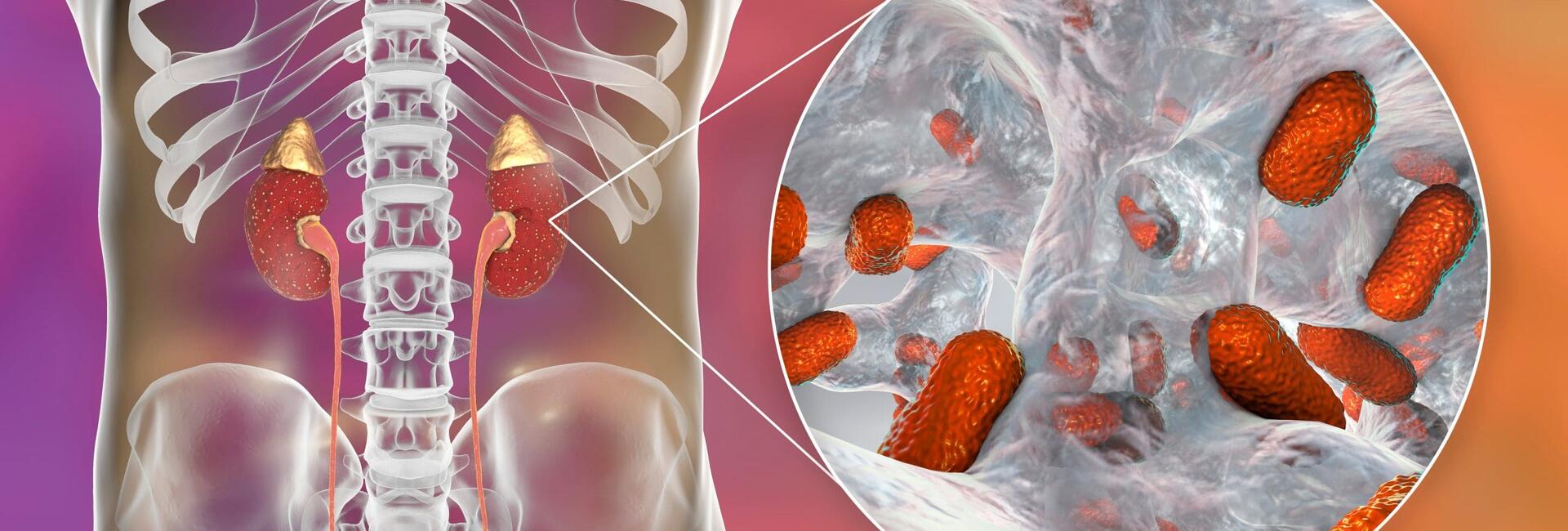
Pyelonephritis is an acute or chronic infectious inflammation of the kidney tissue and its collecting system (bowls, cups). It can be both unilateral and bilateral.
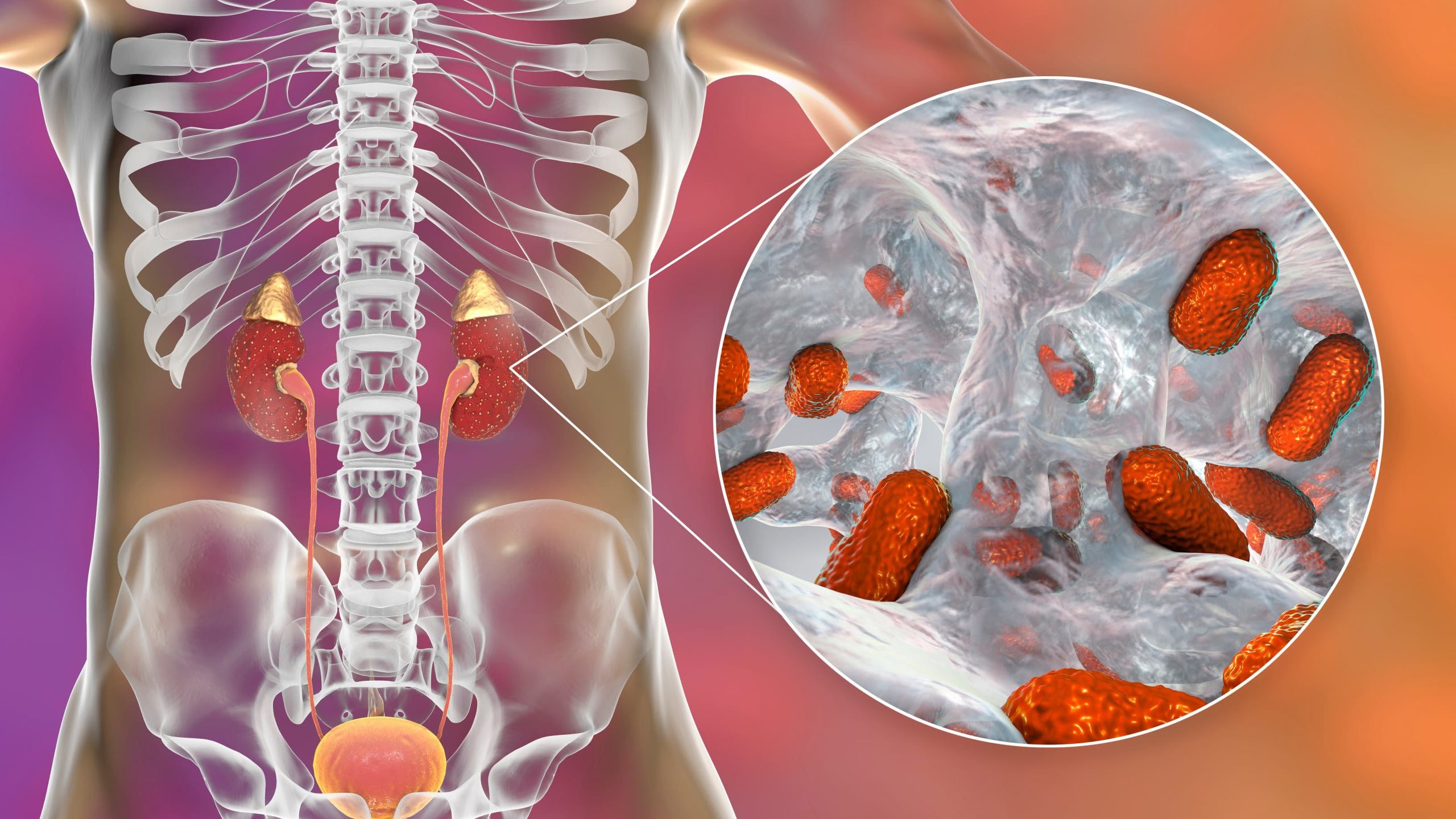
This is the most common disease in urology: pyelonephritis affects people of any age, of both sexes. Women get sick 5 times more often than men, which is related to the anatomical features of the urethra. The probability of the process developing in a child is lower, but it still exists.
Pathology is dangerous because acute inflammation can quickly lead to serious disorders of the function of the kidneys and other organs. Chronic pyelonephritis also does not bode well: the kidney tissue loses a percentage of its functionality after each exacerbation, the risk of developing chronic kidney disease increases.
To avoid dangerous consequences of the disease, pyelonephritis must be treated quickly and correctly. In Kyiv, qualified help can be obtained at the Universum clinic. Consultation of an experienced urologist is also available in Lviv, Khmelnytskyi and other branches of the clinic.
Reasons
The main causative agents are bacteria (Escherichia coli, staphylococci, proteus, streptococci), mycoplasmas, viruses and fungi cause inflammation less often. The infection reaches the kidneys either from the lower urinary tract, as a result of urethritis or cystitis, or is carried by blood from other organs (extrarenal foci).
In a completely healthy person, the bacteria pass through the kidneys in transit or are washed out in the urine. However, this does not always happen.
Common causes of pyelonephritis, which make the body vulnerable to infection:
-
urolithiasis, stones block the outflow of urine, damage tissues, opening the way for microbes;
-
diabetes, gout;
-
impaired blood circulation in the kidneys;
-
anomalies of kidney and urinary tract development;
-
foci of chronic infection (caries, prostatitis, salpingitis, tonsillitis);
-
weakening of immunity (taking corticosteroids, immunosuppressants);
-
attempts to self-treat infections (not only nephrological), which increases the resistance and activity of pathogenic microbes.
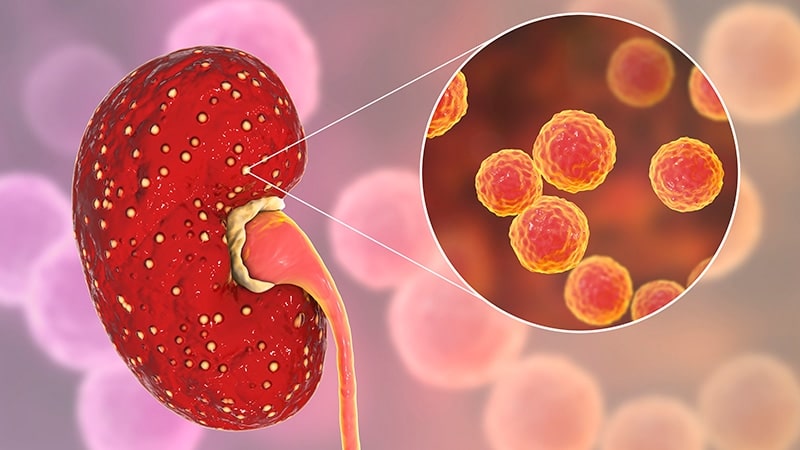
Most often, the causative agent is Escherichia coli. These microorganisms are able to attach to the epithelium of the balls (bowls), which is called the phenomenon of adhesion. Then they begin to colonize the organ, leading to acute, often purulent inflammation.
Why do women get sick more often?
There are several reasons here:
-
a short and wide urethra, which the infection easily overcomes;
-
frequent gynecological diseases and bladder infections;
-
pregnancy, because the enlarged uterus displaces the organs of the abdominal cavity and interferes with normal urination;
-
postpartum weakening of immunity in the case of pathology of pregnancy or childbirth.
Also, women often suffer from chronic salpingitis, salpingo-oophoritis. Pathogenic microorganisms from foci in the pelvis can penetrate the kidneys and cause infectious inflammation.
Types of disease
Depending on the risk factors in an individual patient, pyelonephritis can be primary (on the background of a healthy urinary system) or secondary, as a result of cystitis, urolithiasis.
The course is acute or chronic, and the process tends to become chronic. One of the reasons for this is bacterial associations: several different pathogens are often detected in one patient. When treatment of pyelonephritis is carried out unqualifiedly or at home, this phenomenon is not taken into account, due to which the disease becomes chronic.
Symptoms
Manifestations of the disease depend on the nature of the course of the process, on the accompanying pathology and the general condition of the patient.
Symptoms of acute pyelonephritis:
-
sudden onset;
-
temperature rise to 39–40 degrees;
-
pronounced weakness;
-
chills;
-
nausea;
-
pain in the lower back on the right or left (in case of unilateral acute pyelonephritis) or girdle pain (in case of bilateral);
-
cloudy urine, with pus impurities (the appearance of meat slops may not appear immediately, but on the 3rd-5th day of the disease, when serous inflammation turns into purulent).
Retention of urine, deterioration of urination during an uncomplicated process is rare. If a person suffers from urolithiasis, which increases the risk of bacterial inflammation, urination from the affected kidney may stop. A decrease in the volume of daily urine is a sign of the seriousness of the disease, such people need urgent help.
Chronic pyelonephritis more often occurs as a result of a deficient acute, although it sometimes occurs as a primary process. Symptoms of this variant of the disease often do not attract attention:
-
weakness;
-
subfebrile temperature (up to 37.5 degrees);
-
dull pain in the side on the side of the affected kidney;
-
deterioration of appetite;
-
dysuria (disorders of urination - urges become more frequent or less frequent, night wakings).
During the period of remission, the patient is unlikely to monitor the listed manifestations. And when the exacerbation phase comes, the symptoms accompanying acute pyelonephritis, listed above, appear.
Diagnostics
According to the clinical manifestations, it is impossible to establish a diagnosis of either acute or chronic pyelonephritis. In addition, many patients may have an atypical picture of the disease. For example, with urolithiasis, a kidney infection can resemble renal colic, and people with diabetes do not have a very high temperature.
To diagnose pyelonephritis, the following are performed:
-
medical survey and examination;
-
urine tests, microscopy and bacpos;
-
clinical and biochemical blood tests;
-
blood culture for sterility;
-
Ultrasound of kidneys, pelvic organs and urinary system;
-
radiopaque techniques, including CT;
-
sometimes it is necessary to use radioisotope methods.
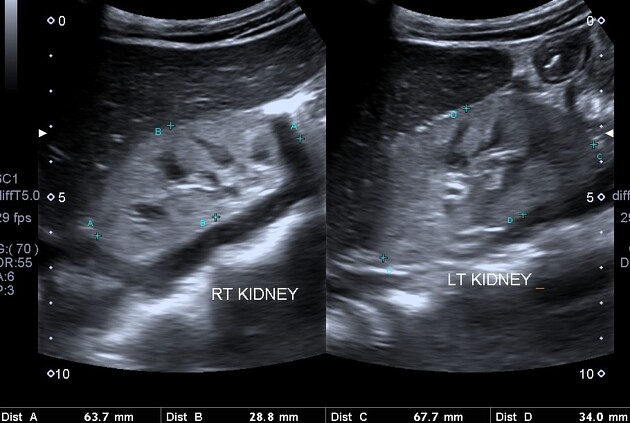
If ultrasound or CT finds signs of blocking the outflow of urine from the kidney, endoscopic diagnosis - cystoureteropyeloscopy - may be necessary. Through the urethra, a thin catheter is inserted into the bladder and ureter, it reaches the renal pelvis and removes the block. Therefore, immediately at the stage of diagnosis, it is possible to carry out a treatment procedure.
Treatment
As a rule, therapeutic methods are used, but sometimes there is a need for surgical intervention.
For the treatment of uncomplicated pyelonephritis, the following are used:
-
antibiotics, which are mainly excreted by the kidneys, drugs are selected based on the results of urine culture (those to which pathogens have retained sensitivity are prescribed);
-
antispasmodics;
-
anti-inflammatory;
-
detoxification therapy using intravenous infusions.
The scheme is drawn up individually, taking into account the causes of the disease (remediation of caries, treatment of sinusitis, salpingo-oophoritis and other foci of infection in the body). At the Universum clinic, if necessary, consultations of the necessary doctors are organized - a gynecologist, an ENT doctor and other specialists.
For the successful treatment of complicated or secondary pyelonephritis, invasive interventions are necessary: catheterization of the ureter, imposition of a nephrostome for urine outflow.
The main thing is to prevent the disease from causing irreparable damage to the kidneys and the body, to avoid the transition to a chronic form and to prevent kidney failure.
The diet for pyelonephritis should provide the body with energy and compensate for protein losses. Non-carbonated water is recommended without restrictions (if the urine passes normally), a lot of easily digestible carbohydrates and proteins. It is not necessary to reduce salt intake if urine flow is preserved.
Thanks to access to modern methods of diagnosis and monitoring, patients of Universum clinic in Kyiv and other cities of Ukraine get the opportunity to completely cure pyelonephritis. With laboratory confirmation of recovery.
Prevention
The main direction is to protect a person from risk factors that increase the likelihood of getting sick. For the prevention of pyelonephritis, it is recommended:
-
avoid hypothermia;
-
carefully follow the rules of hygiene;
-
use condoms during sexual intercourse;
-
be periodically examined for urolithiasis;
-
maintain optimal immune status;
-
contact specialists for timely treatment of urinary tract infections.
These measures will help reduce the risk of primary acute pyelonephritis and protect against exacerbation if the process is chronic.
Rehabilitation
After a course of treatment for acute pyelonephritis with laboratory confirmation of recovery (sterile urine), rehabilitation is minimal. The doctor selects physical therapy exercises, perhaps physiotherapeutic procedures will be useful.
If surgical interventions were performed, rehabilitation measures are based on the surgeon's recommendations.
In the chronic form of the disease, it is recommended to consult a urologist three times a year, undergo an ultrasound examination, and pass urine and blood tests.
Phytotherapeutic treatment courses are useful for consolidating the achieved successes. What drugs to take and for how long - the urologist of the clinic will tell you in detail.
Sources
- Castaigne J, Georges B, Jouret F. Vignette diagnostique de l’étudiantLa pyélonéphrite aiguë [Acute pyelonephritis]. Rev Med Liege. 2022 Sep;77(9):544-547. French. PMID: 36082603.
- Сlinical Practice Guidelines for the Antibiotic Treatment of Community-Acquired Urinary Tract Infections Cheol-In Kang1Infect Chemother. 2018 Mar; 50(1):67-100. English.
- Pierce C, Keniston A, Albert RK. Imaging in Acute Pyelonephritis: Utilization, Findings, and Effect on Management. South Med J. 2019 Feb;112(2):118-124. doi: 10.14423/SMJ.0000000000000936. PMID: 30708379.
- Pietrucha-Dilanchian P, Hooton TM. Diagnosis, Treatment, and Prevention of Urinary Tract Infection. Microbiol Spectr. 2016 Dec;4(6). doi: 10.1128/microbiolspec.UTI-0021-2015. PMID: 28087935.
F. A. Q.
-
acute - the temperature rises sharply to 39-40 degrees;
-
hurts in the side, in the area of the kidney on one or both sides;
-
is haunted by a feeling of weakness, brokenness, lethargy and apathy;
-
headache, chills;
-
want of go for a little more often or less often than usual, urine is like meat slop (turbid, with an admixture of pus);
-
without treatment, within 2-3 days the symptoms increase to complete exhaustion and sepsis;
-
the chronic process in the stage of remission almost does not manifest itself;
-
the best way to understand the diagnosis is a consultation with a urologist and examination.
-
this is an infectious inflammation of the kidney balls, cups and tissues of the organ;
-
at first, the inflammation is serous, but after 2-3 days it can become purulent;
-
there is a threat of the formation of an abscess or carbuncle of the kidney;
-
severe necrotic, emphysematous, apostematous forms of the disease may develop;
-
the most unfavorable result is pyonephrosis, when the kidney tissue melts into pus completely, the organ dies;
-
with bilateral damage, acute renal failure may develop;
-
the purulent process can lead to the death of a person due to endotoxic shock, intoxication;
-
with a chronic course, the risk of stone formation increases.
-
treatment of an uncomplicated case takes 7–14 days;
-
in the case of a severe course, the duration of therapy and rehabilitation may be extended for several weeks;
-
without treatment, the disease either progresses and in 3–5 days forces a person to seek emergency help, or in 7–10 days it subsides a little and turns into a chronic process.
-
this is an infectious inflammation, but the disease is not contagious;
-
the most common pathogens are Escherichia coli, Klebsiella, Proteus, staphylococci and streptococci;
-
the infection enters the kidneys either through the ureter, due to untreated cystitis, or is carried by blood from foci in other human organs;
-
the risk of getting sick is greater if the rules of sexual and personal hygiene are not observed (due to the fact that the probability of introducing an infection into the genitourinary system increases).