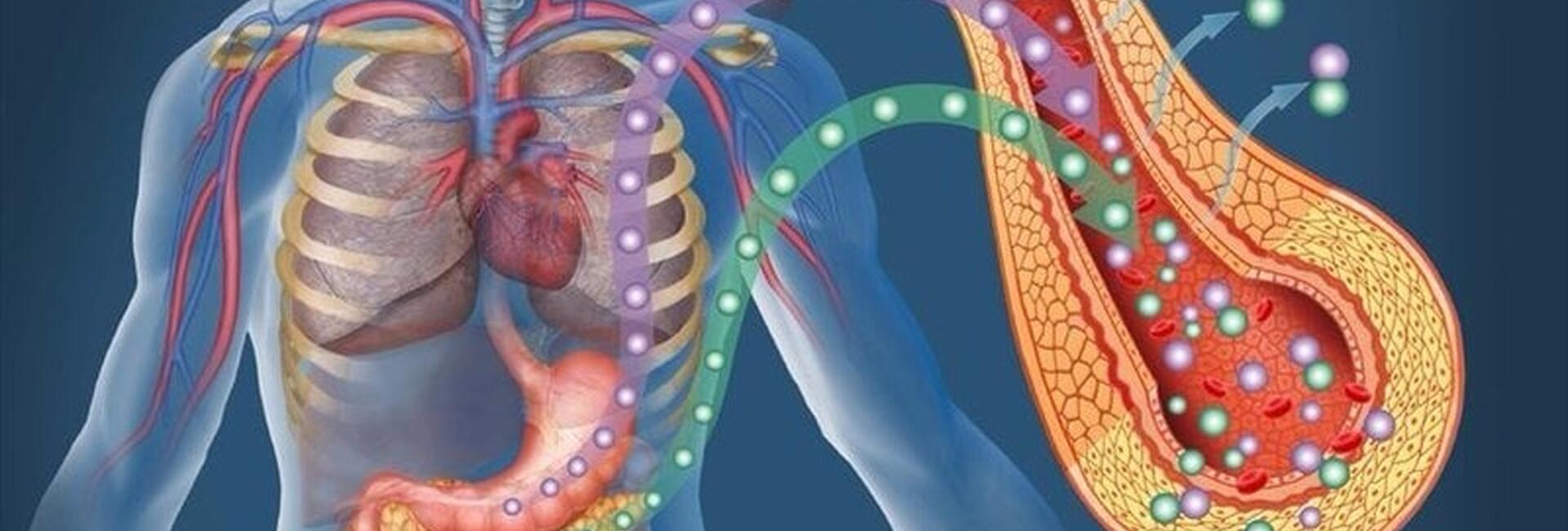
Diabetes mellitus (DM) is a chronic disease associated with persistent elevated blood glucose levels. The danger is not only hyperglycemia, but also its long-term consequences: polyneuropathy, severe microcirculatory disturbances, acute metabolic disorders. It is not for nothing that diabetes mellitus is one of the three most disabling diseases.
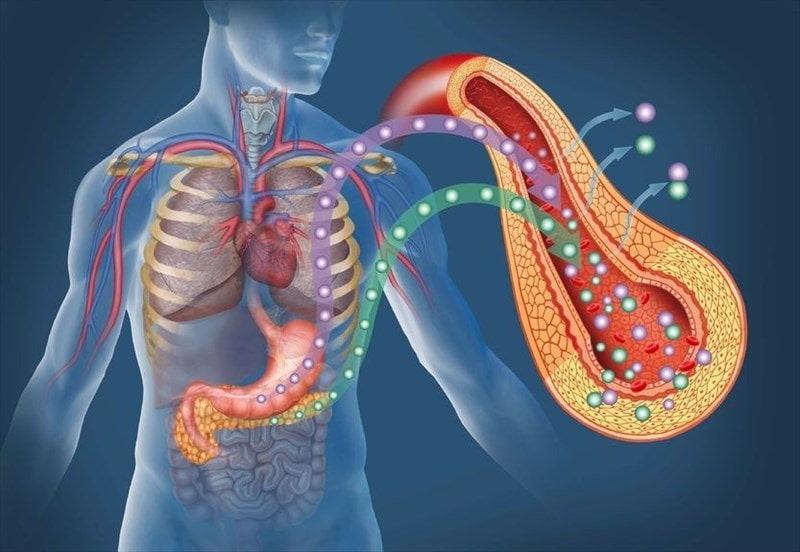
At the same time, the help of a qualified endocrinologist can compensate for the destructive effect of the disease on the body. Consultation with a doctor at the LuxMedic Clinic will help diagnose diabetes mellitus, determine its type and severity, and choose the optimal therapy.
Causes
The mechanism of diabetes development is well understood, which allows doctors to control the course of the disease.
In the pancreas there are islets of cells that synthesize the hormone insulin. This is the substance without which glucose from the blood cannot enter the cells of the body (except for neurons - the brain does not need insulin).
Two situations can lead to the development of diabetes mellitus:
-
Insufficient production of insulin. There is not enough of the hormone to reach all the tissues. As a result, sugar is simply not used by the muscles, and its level in the blood rises. This condition is called type 1 diabetes mellitus.
-
Deterioration of the active production of the hormone of necessity (type two). In absolute terms, the hormone is synthesized in normal amounts. But when a person eats, there is no rapid increase in production (postprandial peak). The result is the same: insulin deficiency, hyperglycemia.
Knowing these mechanisms and determining what type of diabetes mellitus a particular patient has is extremely important: treatment tactics depend on it.
Provocative Factors
The main causes that can lead to persistent hyperglycemia in humans are also known.
Type 1 diabetes mellitus is more commonly provoked by the following factors
-
Genetic predisposition to impaired insulin synthesis
-
Stress
-
Viral infections
-
Autoimmune destruction of pancreatic islet cells;
-
Acute or chronic pancreatitis with pancreatic necrosis, tissue fibrosis;
-
Injury and surgery resulting in loss of pancreatic tissue.
The first type of the disease, insulin-dependent, is more common in young men and women and can develop in children and adolescents.
Type 2 (non-insulin-dependent) diabetes develops for other reasons:
-
Hereditary resistance of cell receptors to insulin perception;
-
Obesity, often accompanied by chronic inflammation;
-
Improper diet with carbohydrate overload.
As a result, as type 2 diabetes progresses, the secretory function of the islet cells also weakens. This type of disease is characteristic of the elderly.
Diabetes Symptoms
The classification of diabetes is broad and complex. Although it takes into account the severity of the disease, it is more useful to clinicians. Simply put, there are several stages in the development of the disease, which are manifested by different symptoms.
The first stage is impaired glucose tolerance. This is usually the beginning of type 2 diabetes. The problem can only be noticed when you test your glucose level after a meal: it will be elevated. Over time, noticeable symptoms develop:
-
thirst, a person drinks a lot of water;
-
polyuria, frequent urination to the toilet
-
slimming, body slimming;
-
weakened immunity, frequent urinary tract infections;
-
wounds and skin lesions take a long time to heal;
-
abdominal discomfort and pain, diarrhea
-
visual disturbances;
-
kidney dysfunction, edema;
-
spots on the skin;
-
cold feet and hands;
-
decreased sensation in the skin of the extremities.
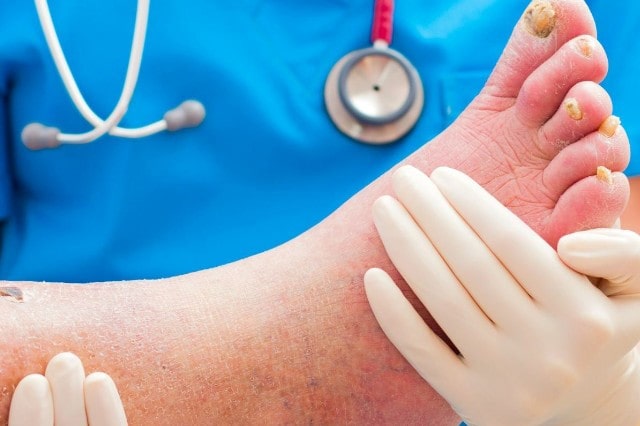
Due to high glucose levels, carbohydrates are incorporated into enzyme molecules and cell membranes, and they can no longer function properly. As a result, the function of capillaries (diabetic angiopathy) and nerve fibers (polyneuropathy) is impaired. The heart muscle, kidneys, and liver are affected, and the blood supply to the extremities is impaired.
Emergency conditions
In addition to the slow progression of the disease, acute metabolic disorders may occur: ketoacidotic coma, osmolar coma, etc.
The danger is manifested by depression of consciousness, a person is apathetic, lost, and may vomit. The breath smells like wet apples (ketoacidosis is common in children).
Any impairment of consciousness, especially if a person is aware of glucose problems, requires emergency medical care.
Diagnosis
A very important point. Despite the availability of diagnostics, many patients do not turn to suspected diabetes mellitus, whose symptoms are not noticeable, but in advanced stages of the process.
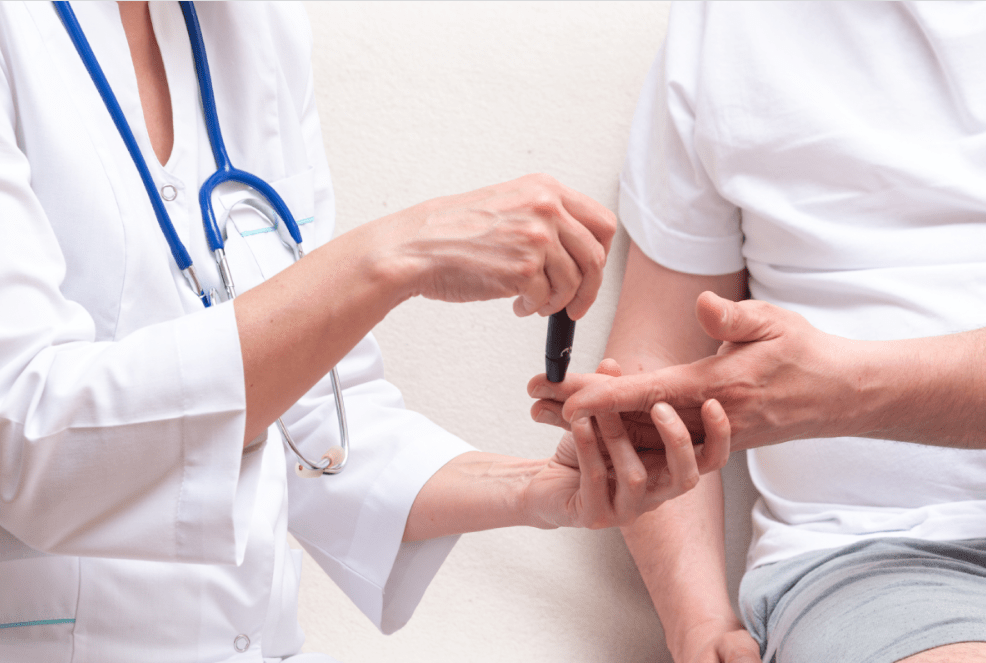
A consultation with an endocrinologist at the LuxMedic Clinic can help determine within a few minutes whether a person is at risk of developing diabetes. If necessary, a more detailed examination will be carried out:
-
Determination of fasting and postprandial blood glucose levels;
-
Carbohydrate tolerance tests;
-
Urine tests for sugar excretion;
-
Glucose impregnated (glycosylated) hemoglobin levels;
-
C-peptide levels, which indicate pancreatic islet cell function.
In doubtful cases, the list of tests can be expanded. Often it is necessary to evaluate the lesion of other organs: ECG, ultrasound of heart, liver, kidneys. If necessary, the clinic organizes a consultation with a neurologist, ophthalmologist, therapist.
Diabetes Treatment
Only a specialist can select an appropriate therapy that will allow you to maintain normal blood sugar levels and not cause carbohydrate deficiency, hypoglycemia.
The general principles of treatment of diabetes mellitus are as follows
-
Strict diet with restriction of carbohydrate intake;
-
Use of tablet preparations that either increase insulin secretion or sensitize cell membranes to this hormone (insulin-independent variant);
-
Over time, the pills may stop working (relevant to type 2 disease), the process becomes secondary insulin dependent;
-
Use of short-acting and long-acting insulin preparations;
Treatment of complications that have developed as a result of the disease.
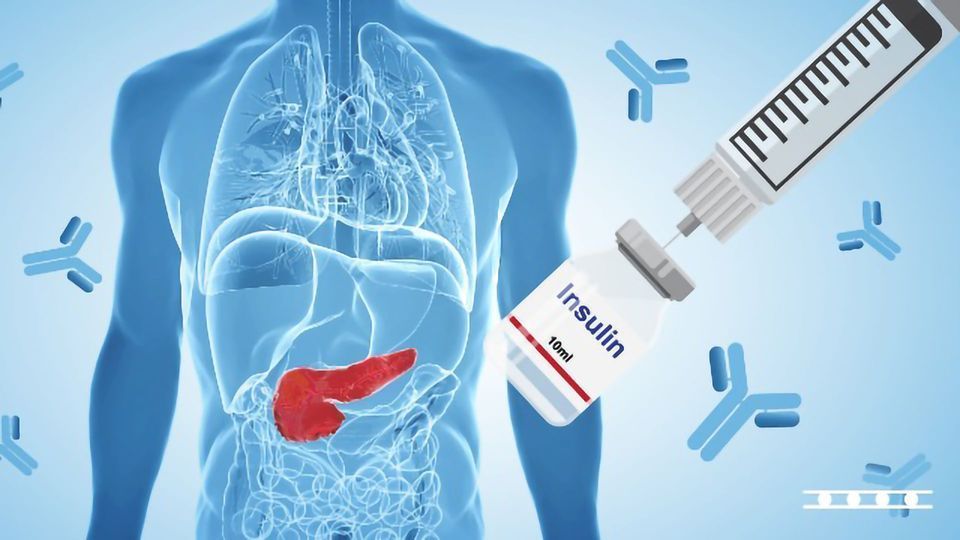
Patients with confirmed diabetes mellitus should start treatment with regular blood glucose monitoring. A specialist of LuxMedic Clinic will help to organize the control, will explain in detail the basic rules of nutrition and will teach how to calculate the optimal dose of insulin therapy.
In advanced cases it is necessary to consult external specialists: surgeon, ophthalmologist, cardiologist, nephrologist.
The effectiveness of therapy is confirmed by periodic examinations. There should be no glucose in urine, the indicator of glycosylated hemoglobin should return to a normal level.
Thanks to qualified treatment, diabetes mellitus passes to the stage of compensation and does not have a harmful effect on the human body for decades.
Prevention
Risk factors should be avoided. Eat right, fight stress, maintain immunity to resist viral infections. Physical activity is important: fats are broken down, tissue sensitivity to insulin increases.
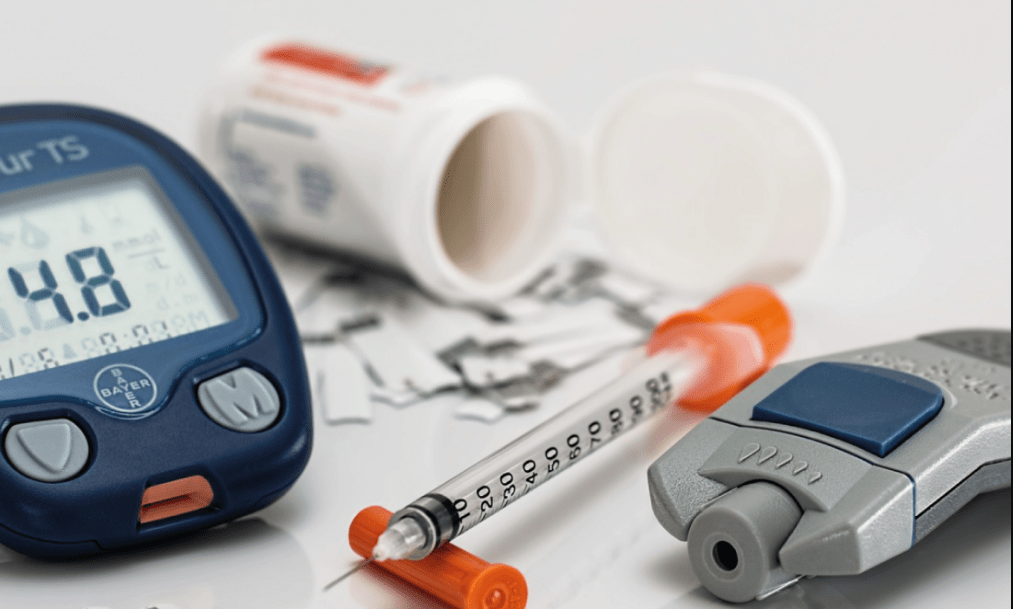
The best way to prevent diabetes mellitus is to monitor your blood sugar levels regularly. An annual check-up can nip the disease in the bud at the stage of impaired glucose tolerance. This will give doctors the opportunity to make a plan to prevent the progression and development of complications of the disease. And in the early stages it is enough to change dietary habits.
Rehabilitation and Nutrition
In a disease such as diabetes mellitus, diet is the key to a person's successful treatment. The diet is prepared so that the caloric intake from food correlates with the energy needs of the body. The calculation of the energy rate is done individually for each patient.
General dietary advice for diabetes mellitus:
-
5-6 meals a day, in small portions;
-
Calorie distribution for each meal;
-
Careful calculation of the number of conventional bread units in each portion;
-
Alcohol is prohibited as it can lead to hypoglycemia, ketoacidosis;
-
More fiber-rich foods (e.g., sprouted grains) should be included in the menu;
-
Low-calorie vegetables, salads, cabbage, squash, legumes, tomatoes;
-
Fat-free meat broths are allowed;
-
lean poultry, fish (perch, flounder, cod, pike), crayfish;
-
as spices - onion, pepper, horseradish;
-
Drinks - decaffeinated coffee, barley drinks, tea, mineral water.
It is better to steam or grill it to reduce the amount of fat. Each portion should be weighed to correctly calculate bread units.

Physical activity is always beneficial in type 2 diabetes: walking, running, light exercise. For patients with DM 1, physical activity must be dosed because the risk of hypoglycemia increases.
Since the disease is considered chronic, there is no need for rehabilitation. However, if you contact the clinic in time, the doctor at the LuxMedic Clinic will help you normalize your blood sugar and give you recommendations on how to keep it normal for years to come. In this way we will save a person from the negative impact of the disease on life and health.
Sources
-
Ministry of Health of Ukraine, "Cerebral diabetes, clinical guidelines based on evidence", dated 26.01.2023.
-
American Diabetes Association. Diagnosis and Classification of Diabetes Mellitus. Diabetes Care. 2011 Jan;34 Suppl 1(Suppl 1):S62-9. doi: 10.2337/dc11-S062. PMID: 21193628; PMCID: PMC3006051.
-
Theivasigamani K, Palaniappan S. A review of pharmaceutical care in patients with type II diabetes mellitus: Current Position and Perspectives. Curr Diabetes Rev. 2023 May 5. doi: 10.2174/1573399819666230505123428. Epub ahead of print. PMID: 37151063.
-
Michaelidou M, Pappachan JM, Jeeyavudeen MS. Diabetes management: Current concepts. World J Diabetes. 2023 Apr 15;14(4):396-411. doi: 10.4239/wjd.v14.i4.396. PMID: 37122433; PMCID: PMC10130896.
-
Zaino B et al. Diabetic neuropathy: Pathogenesis and evolving treatment principles. Dis Mon. 2023 May 8:101582. doi: 10.1016/j.disamonth.2023.101582. Epub ahead of print. PMID: 37164794.
F. A. Q.
-
At the very early stage, when glucose tolerance is impaired, there are no symptoms of pathology;
-
The best way to detect the beginning of the process is to be examined in the clinic, quick diagnosis takes a few minutes.
-
Frequent feelings of hunger and thirst;
-
Episodes of dizziness;
-
Deterioration of general well-being after eating (postprandial);
-
As the disease progresses, polyuria, recurrent infections, chronic fatigue syndrome, poor healing of skin wounds;
-
Women often have inflamed genitals (glucose is excreted with urine, remains on the genitals and serves as a breeding ground for bacteria);
-
Cold feet, dry and pale blue skin on the extremities;
-
Skin sensitivity in the feet and toes is impaired.
-
If the problem is detected in time, it is possible to normalize carbohydrate metabolism;
-
In the case of advanced DM, a person will need ongoing supportive treatment to control blood glucose levels.
-
Do not try to lower blood sugar on your own, as this can lead to severe hypoglycemia or ketoacidotic coma;
-
Normalize blood glucose gradually, in contact with a doctor;
-
Overdose of glucose-lowering medications should be avoided;
-
The risk of a rapid drop in blood glucose and complications is increased by alcohol consumption and, in type 1 diabetes, by physical exertion.