Vaginitis is a medical term that describes various disorders that cause vagina to become infected or inflamed, a synonym for it is colpitis. The disease is widespread: every third woman on the planet faced with it. Little girls, adults and elderly women can get infected. Vaginitis has a variety of types and causes, that’s why a professional individual approach to each patient is required for effective treatment.

Symptoms of vaginitis
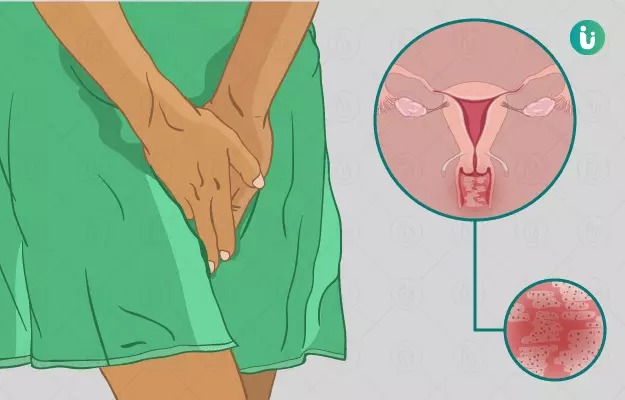
Inflammation of the mucous membrane of the vagina manifests itself with quite characteristic signs.
The LuxMedic Clinic gynecologist recommends to pay attention to the following symptoms, which are characteristic for vaginitis:
- increase the amount of vaginal discharges;
- itching inside and near the entrance to the vagina;
- feeling of burning in the lower abdomen, redness of the skin in the area of the labia;
- frequent urination;
- pain and discomfort during sex (dyspareunia);
- bleeding;
- rise of the temperature and deterioration of well-being.
If at least one of the above-mentioned signs appears, you should have a consultation with gynecologist, since different types of the disease manifest themselves in different ways. For example, atrophic vaginitis has such symptoms as excessive dryness of the vagina and disappearance of discharges.
Classification of vaginitis
Having discovered unpleasant symptoms, some women can try home treatment, using advice from the Internet or recommendations from friends. Home treatment of vaginitis is not recommended: effective home treatment of the disease is impossible if nature, type, clinical variant of vaginitis is not taken into account.
Colpitis are devided by its origin:
- Specific ones caused by sexually transmitted infections (STIs).
- Non-specific etiology caused by other flora and non-infectious factors.
According to the nature of the course:
- Acute vaginitis with relatively violent clinical picture and symptoms.
- Subacute, with manifestations up to 3 months old.
- Chronic (the symptoms are not so clearly manifested and last longer than 3 months.
- Asymptomatic form of the disease. A woman does not feel any signs of the disease, but during a gynecological check up deviations from the bacterial flora of the vagina are found. This condition is extremely dangerous for expectant mothers.
It is very important to determine correctly the origin of vaginitis. For effective treatment, it is necessary to define the cause of the vaginitis and eliminate it.
Causes of vaginitis
Most often, women with infectious processes need consultation with gynecologist. The most common factor is pathogenic flora:
- trichomonads;
- chlamydia;
- gonococci;
- fungi of the Candida genus;
- genital herpes;
- enterococci;
- staphylococci;
- escherichia coli;
- gardnerella.
In the case of infectious inflammation, there is a combination of various pathogenic microorganisms. This needs attention, professionaltherapy and control in order to cure colpitis and not turn it into a chronic form.
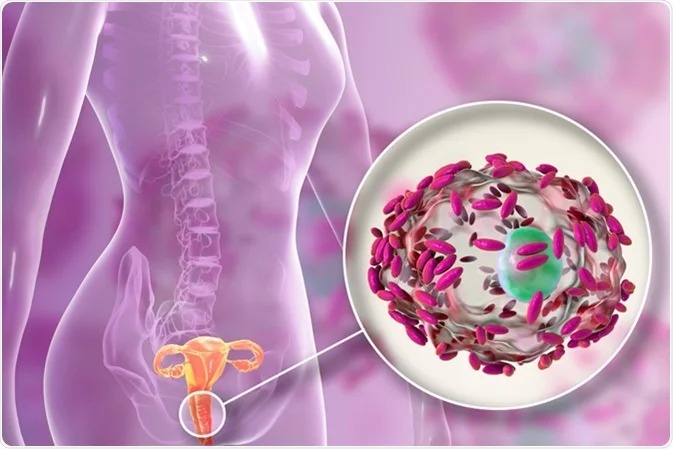
The list of causes of non-infectious vaginitis includes the following factors:
- atrophy of the mucous membrane due to hormonal disorders (menopause, use of inappropriate drugs and contraceptives);
- allergic reactions to latex, vaginal creams, ointments;
- traumatization of the epithelium, for example, by toys for adults;
- non-genital pathology (Behcet's disease, diabetes);
- thermal influence (hot baths, shower);
- irritation with vaginal hygiene products.
And some other pathological conditions.
A frequent but not obvious cause of infectious colpitis is the use of antibiotics. As a result, the physiological microflora (lactobacilli) dies and bacterial vaginitis develops.
Why is vaginitis dangerous
First of all, non-infectious inflammation reduces the quality of life. In addition, the following problems are possible:
- problems with conception;
- vaginal scarring;
- formation of fistulas (pathological channels between the vagina and neighboring organs).
Complications of the infectious process are associated with the spread of infection to the internal genital organs (cervicitis, salpingitis, endometritis) and urinary tract (cystitis, pyelonephritis). There are also risks for conception and pregnancy.
Methods of diagnosing vaginitis
Every patient with symptoms of colpitis should have a consultation with a gynecologist. A consultation at the LuxMedic Clinic will help define accurate diagnosis quickly and make an individual plan of treatment.
To diagnose and clarify the disease, the following methods are used:
- gynecological examination with mirrors to assess the condition of the vaginal mucosa;
- smear to determine the bacterial spectrum;
- microbiological study of excretions of female genital organs in order to detect the resistance of microbes to antibiotics;
- rapid PCR tests for STI pathogens;
- PIF - direct immunofluorescence for suspected chlamydia;
- measuring the pH of the vaginal contents allows you quickly distinguish whether it is a microbial process and a non-infectious one.
In order to rule out complications, especially if vaginitis is chronic, ultrasound of the pelvic organs is recommended. Some patients may need blood, urine and other tests additionally. According to the results of the tests, the cause, form, and variant of the course of the disease are made. After that, we make an individual treatment plan for the woman.
Treatment of vaginitis
Therapy should be prescribed only after verification of the diagnosis and clarification of all the nuances of the disease. Otherwise, vaginitis will progress and cause complications.
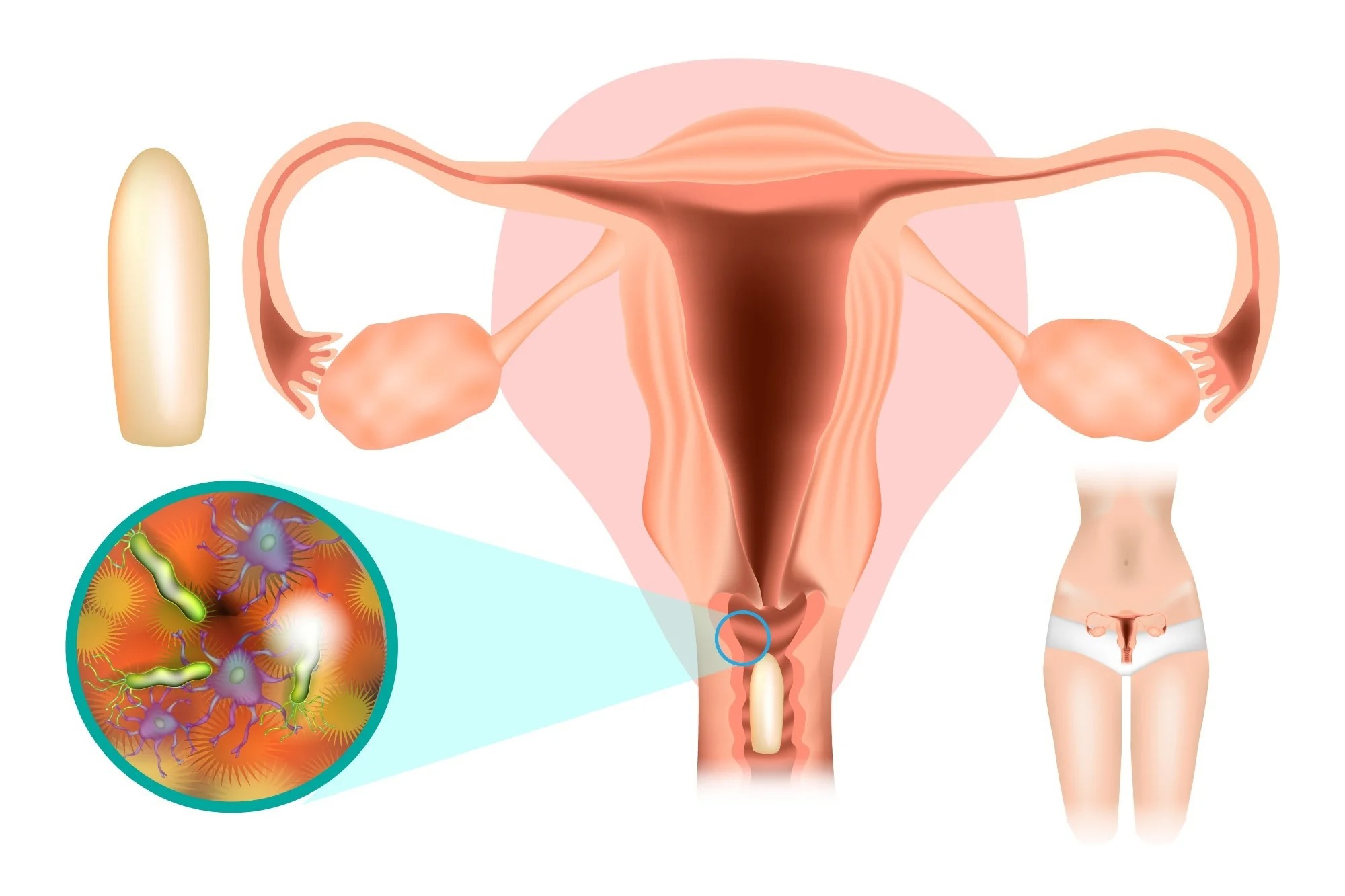
Treatment is strictly pathogenetic:
- in case of detection of STDs or other infections - antibiotics srevprescribed based on results of the tests, antimicrobial agents;
- candida - antifungal drugs;
- atrophic processes - normalization of hormonal balance;
- treatment of extraneous pathology, complications
If necessary, immunomodulators and probiotics are added. We combine systemic therapy and methods of local treatment of vaginitis.
To eliminate the cause of the disease we make consultations of related specialists, for example, an endocrinologist for diabetes treatment. If the girl has a disease, it is recommended to have a consultation with pediatric gynecologist.
Often one woman has several factors that cause inflammation. Therefore, for each LuxMedic Clinic’s patient, a treatment plan is made individually, and recovery is confirmed by a doctor's examination and laboratory tests.
Prevention of vaginitis
General recommendations are made to maintain health:
- observance of sexual hygiene;
- underwear should be made of natural fabric, cotton;
- protected sexual contacts;
- active lifestyle;
- balanced nutrition;
- do not treat vaginitis at home.
Girls and women are recommended to undergo annual gynelogical check up, even if there are no negative symptoms. Woman should get examined before planning a pregnancy. This will make it possible to detect and treat asymptomatic forms of pathology with dangerous complications.
Literature
- Egan ME, Lipsky MS. "Diagnosis of vaginitis.", Am Fam Physician. 2000 Sep 1; 62 (5): 1095–104. PMID: 10997533.
- Sherrard J. "European guideline for management of vaginal discharge.", International Journal of STD & AIDS. 2001; 12 (2_suppl): 73–77. doi:10.1258/0956462011923985
- Surbone A et al. "Microbiote vaginal et vaginose [Vaginal microbiota and vaginosis]". Rev Med Suisse. 2022 Oct 19;18(800):1941–1949. French. doi: 10.53738/REVMED.2022.18.800.1941. PMID: 36259699.
- Nyirjesy P. "Management of persistent vaginitis.", Obstet Gynecol. 2014 Dec;124(6):1135–1146. doi: 10.1097/AOG.0000000000000551. PMID: 25415165.
F. A. Q.
- sexually transmitted infections;
- non-specific bacterial microflora;
- fungi and viruses;
- decrease in the level of estrogens in the blood;
- intrauterine spiral;
- physical factors - chemical, temperature, trauma to the epithelium of the vagina;
- antibiotics and corticosteroid hormone preparations;
- immunodeficiency states;
- insufficient or excessive hygiene of the genital area.
- 2 times a year or more often there are complaints of itching, burning, dyspareunia;
- discharge from the vagina, as a rule, more abundant than usual;
- white ones have an unpleasant smell;
- manifestations are wave-like: they periodically intensify and weaken.
- a center of chronic infection is formed in the body;
- the quality of life deteriorates;
- the risk of cervicitis, endometritis, salpingitis and cystitis oophoritis, pyelonephritis increases significantly;
- there are problems with conception and pregnancy.
- infectious and non-infectious;
- acute, subacute and chronic;
- asymptomatic, when nothing bothers you, but the risks for pregnancy and the health of other organs remain.







