Trichomoniasis (or trichomonosis) is one of the sexually transmitted infections (STIs). This infection is prevalent and can affect both men and women. The causative agents, known as trichomonads (Trichomonas vaginalis), belong to the category of protozoa with flagella, which makes the diagnosis and treatment of trichomoniasis unique.
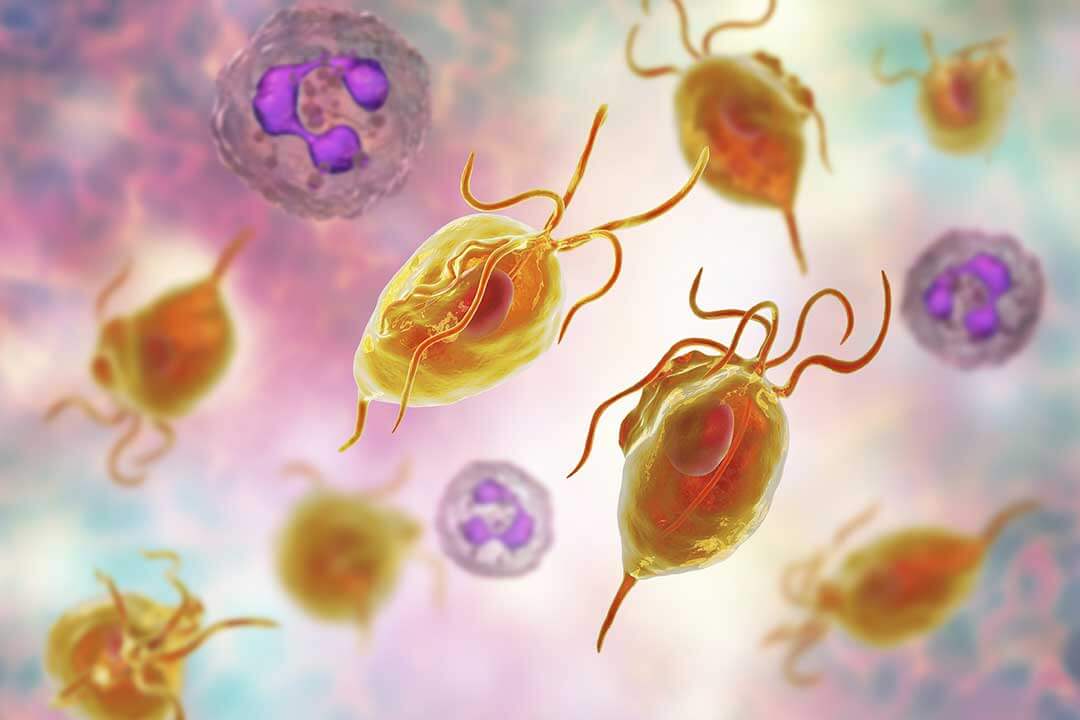
Specifically, this infection is not susceptible to antibiotic treatment. Moreover, these human pathogens can harbor other STI agents such as gonococci and chlamydia. Consequently, if trichomoniasis is treated incorrectly, recurrences of venereal diseases often occur.
Types of Trichomoniasis
Like other venereal infections, trichomoniasis can have various clinical courses in dermatovenereology:
-
Acute, occurring within 2 months of infection.
-
Chronic, with an infection duration exceeding 8 weeks.
-
Latent (asymptomatic trichomonad carriage).
To assess the activity of the disease, acute trichomoniasis is further categorized into three phases:
-
Acute phase, with pronounced and noticeable symptoms.
-
Subacute variant, with mild or vague manifestations.
-
Torpid inflammation, where the pathogens are present in the body but do not manifest.
Based on the severity of the condition, trichomoniasis is classified as complicated or uncomplicated.
The torpid and subacute course of the disease often leads to the development of chronic trichomoniasis. It is mainly individuals with such mild symptoms who contribute to the spread of venereal infections without realizing it.
Due to this unique feature, periodic check-ups with a dermatovenerologist are highly recommended. At LuxMedic Clinic, one can undergo anonymous testing for trichomoniasis and other STIs, thus protecting their loved ones from infection and themselves from complications of the disease.
Pathogenesis and Symptoms of Trichomoniasis
This disease exhibits several characteristics that experienced dermatovenereologists are aware of and take into account:
-
High infectivity: Trichomonas vaginalis has specific receptors on its surface, which allow it to bind to human epithelial cells within a few minutes after infection.
-
Significant virulence: Trichomonads destroy red blood cells, reduce the activity of tissue immunity, and create a gateway for other STI agents.
-
Resistance to the immune response: Immune cells are unable to eliminate the pathogens and may perish, leading to a subacute inflammatory process.
-
Propensity for a chronic course: Infections often have subtle, hidden symptoms, but infected individuals can transmit the disease, particularly through unprotected sexual contact.
If left unnoticed or untreated, complications such as adhesions and persistent reproductive organ disorders can arise, and in men, trichomoniasis may even lead to infertility.
Symptoms of Different Forms of Trichomoniasis
The target of pathogenic Trichomonas vaginalis is the epithelial cells of the human genitourinary system. People usually become infected during unprotected sexual intercourse. Microorganisms firmly attach to receptors on the cells of the urethra or vagina within a few minutes and start reproducing.

The incubation period of trichomoniasis is 5-7 days, although it can vary from 3 days to 2 weeks. Afterward, the inflammatory process begins.
Typically, the genitourinary system is affected, but trichomonal infection can also occur in the rectum or oral cavity.
Symptoms in Men
In men, Trichomonas initially affects the urethra and then spreads to other organs of the genitourinary system.
Common signs of the disease include:
-
Urethritis: Burning during urination, frequent urination.
-
Balanoposthitis: Inflammation of the glans and foreskin, pain, spots, ulcers, and an unpleasant odor when retracting the foreskin.
-
Prostatitis: Discomfort in the perineal area, difficulty urinating, thin and weak urinary stream.
-
Vesiculitis and epididymitis: Inflammation of the testicles and their appendages, manifesting as a dull pain in the groin area and scrotum, as well as reduced pleasure during ejaculation.
In some cases, the disease in men may be asymptomatic. In the morning, minimal urethral discharge may be noticed, less than in the case of gonorrhea. There may also be sticky urethral lips in the morning.
Symptoms in Women
The first organ attacked by Trichomonads is typically the vagina.
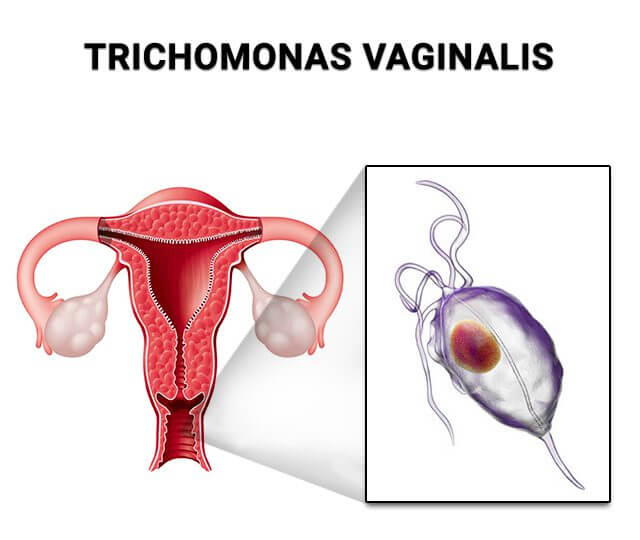
Then, similar to men, the parasites spread through the female genitourinary system.
Symptoms that should raise suspicion of trichomonal infection in women include:
-
Itching, burning, pain near the entrance of the vagina, swelling, and skin ulcers on the genital lips (vulvitis).
-
Swelling near the entrance of the vagina, serous and purulent discharge, and pain (Bartholinitis).
-
Copious, thin, often frothy, pale yellow or yellowish vaginal discharge with an unpleasant odor, sometimes with a hint of blood (colpitis, vaginal inflammation).
-
Pain, itching, and burning in the vagina and lower abdomen (cervicitis and endocervicitis).
-
Menstrual irregularities, varying degrees of lower abdominal pain (endometritis and salpingo-oophoritis).
-
Increased urination frequency, burning, and pain during urination (cystitis).
Sometimes, trichomoniasis in women can manifest with the development of condylomas similar to human papillomavirus infection.
Another characteristic of female trichomoniasis is that it often remains asymptomatic. Even without symptoms, inflammation can persist and, if the fallopian tubes are affected, it can lead to infertility.
Diagnosis of Trichomoniasis
Considering that both men and women often contract trichomoniasis without symptoms, it is recommended to undergo an annual examination by a dermatovenereologist. This is especially crucial for individuals leading an unconventional sexual lifestyle. Women should consider testing when planning a pregnancy or experiencing difficulties in conceiving. Consultation with a specialist is necessary if there are signs of inflammation of the genitourinary organs.
Since trichomonads are protozoa, rather than bacteria, specific diagnostic approaches are required. Specialists at LuxMedic Clinic will select the optimal diagnostic algorithm. Diagnostic methods used in the clinic include:
-
Microscopic examination of tissue samples from the urethra, cervix, and vaginal smears.
-
Culture-based testing, which is a highly accurate but time-consuming method to culture trichomonads on a specialized growth medium.
-
Immunological methods for rapid detection of antibodies in the patient's blood.
-
Immunofluorescence, enzyme-linked immunosorbent assay, and PCR (polymerase chain reaction).
-
Ultrasound examination of the reproductive organs and pelvic region to detect adhesion-related complications of trichomoniasis.
Thorough examination using provocative tests (e.g., with alcohol) allows our doctors to make an accurate diagnosis for the patient and their sexual partner, even in cases of hidden, asymptomatic trichomonad carriage.
Treatment Methods for Trichomoniasis
Since the causative agents belong to the category of parasites, antibiotics are not effective. Antiprotozoal agents must be selected. The choice of the specific medication depends on the results of the tests, which indicate which drugs the parasites are resistant to and which will be most effective against them.
To achieve the desired effect and avoid recurrence, a comprehensive approach is necessary, including:
-
Etiotropic treatment with systemic and local antiprotozoal agents.
-
Immunocorrection.
-
Biostimulants and vitamin supplements.
-
Enzyme preparations for treating adhesions in cases of complicated trichomoniasis.

When trichomoniasis is confirmed through testing, treatment is individually tailored to each person. LuxMedic Clinic's doctor takes into account the patient's gender, age, the form of the disease, the presence of complications, and, importantly, other STIs.
Trichomoniasis Prevention
The primary goal is to minimize the risk of infection. To do this:
-
Avoid casual sexual encounters.
-
Use barrier methods of contraception (condoms).
-
Have a single, faithful sexual partner.
-
In case of a confirmed diagnosis, ensure that sexual partners are examined and, if necessary, undergo a full course of treatment for anyone found to be infected.
For individuals at risk of contracting trichomonad carriage due to their lifestyle, regular testing is advisable to minimize the risk.
Sources
- Edwards, Thomas et al. “Trichomonas vaginalis: Clinical relevance, pathogenicity and diagnosis.” Critical reviews in microbiology vol. 42,3 (2016): 406-17. doi:10.3109/1040841X.2014.958050.
- Bouchemal, Kawthar et al. “Strategies for Prevention and Treatment of Trichomonas vaginalis Infections.” Clinical microbiology reviews vol. 30,3 (2017): 811-825. doi:10.1128/CMR.00109-16.
- Turan Faraşat, Vildan et al. “Comparison of Diagnostic Methods for Detection of Trichomonas vaginalis in Prediagnosed Vaginitis Cases and Its Association with Various Pathogens.” Turkiye parazitolojii dergisi vol. 46,3 (2022): 167-171. doi:10.4274/tpd.galenos.2022.02996.
- Ziaei Hezarjaribi, Hajar et al. “Is There Any Relationship between Trichomonas vaginalis Infection and Male Urethritis Risk?” Interdisciplinary perspectives on infectious diseases vol. 2022 8359859. 6 Sep. 2022, doi:10.1155/2022/8359859.
F. A. Q.
-
Urination is accompanied by itching, burning, and sometimes pain.
-
Women may experience frothy white or yellowish vaginal discharge that increases in volume and has an unpleasant odor.
-
In men, the lips of the urethra can stick together in the morning, and there may be minimal discharge.
-
Inflammation, sores, and ulcers may develop on the genital organs.
-
Difficulty in conceiving a child.
-
Consult a clinic and undergo prompt laboratory testing if any symptoms are present.
-
The source of the infection is a person who is infected or an asymptomatic carrier.
-
The disease can be transmitted during unprotected sex in any form: oral, genital, or anal.
-
Rarely, it can be spread through common household items, towels, washcloths, or dirty hands.
-
Pathogenic microorganisms spread through the genital systems of both men and women.
-
Infection can spread, increasing the risk of infecting close family members and sexual partners.
-
The disease progresses to a chronic form, making it difficult to treat.
-
Trichomonads contain other STI agents and can lead to recurring venereal infections.
-
Acute infection disrupts the functioning of the reproductive system.
-
Chronic, latent inflammation can lead to the formation of a chronic infection focus in the body, increasing the risk of autoimmune processes.
-
The disease can cause severe complications, including tubal infertility, prostatitis, and irreversible testicular dysfunction.







