The endometrial polyp is a benign neoplasm that develops from cells of the inner mucous membrane of the uterus. Such formations occur in many women aged 30-50 years and after menopause and occasionally occur during puberty. They often occur with mild symptoms. And, unfortunately, some types of endometrial polyps have a dangerous risk of transformation into endometrial cancer.
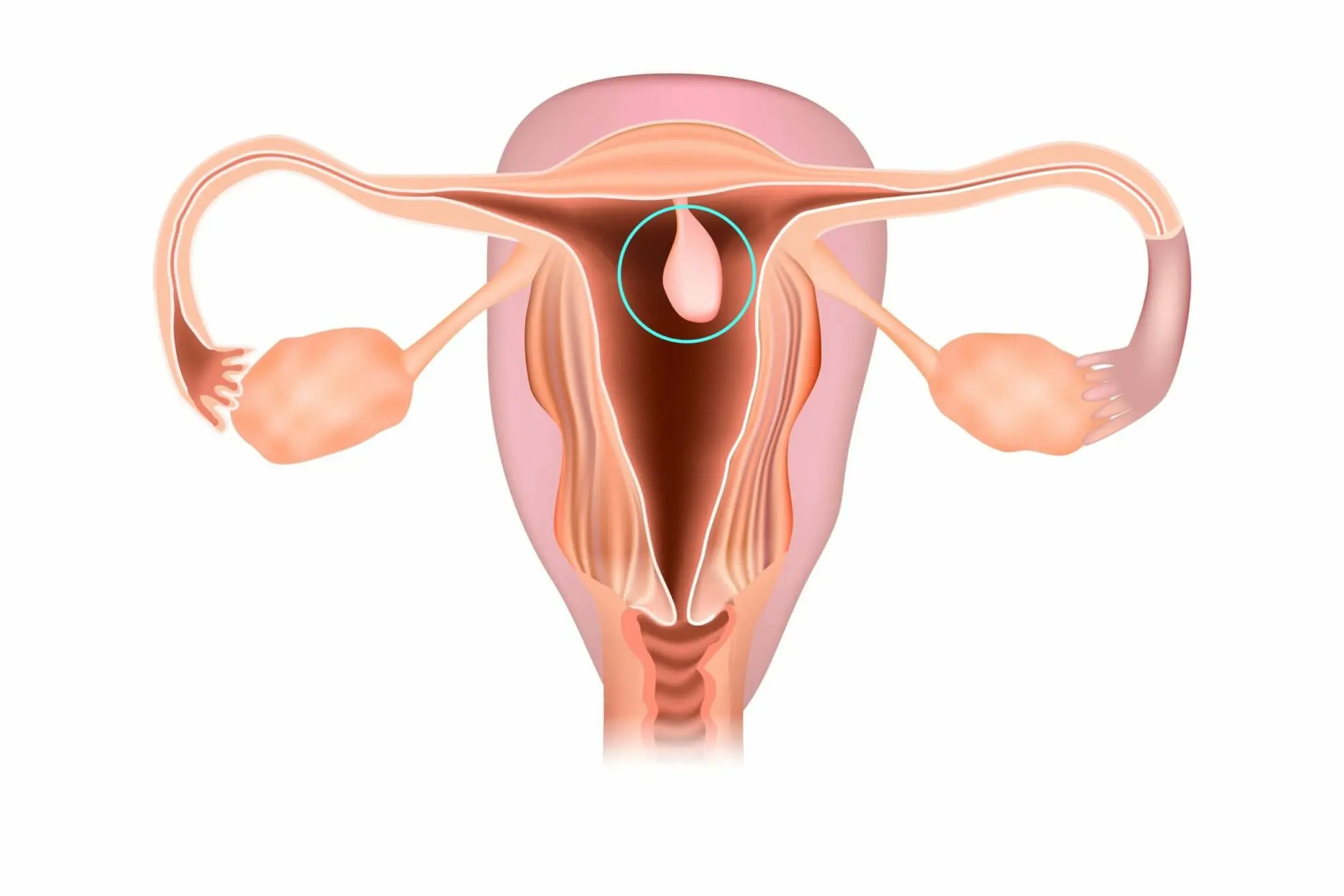
Causes
What exactly leads to the formation of nodes has not yet been established. Nevertheless, doctors know factors that increase the risk of developing pathology:
-
obesity;
-
diseases of the digestive tract;
-
thyroid problems and diabetes;
-
diseases of the cardiovascular system;
-
unprotected sex;
-
polycystic ovary syndrome;
-
uterine fibroids.
Such conditions directly or indirectly disrupt the hormonal balance in the female body and negatively affect the endometrial layer. The inflammatory process in the uterine cavity is essential for the development of polyps. For example, against the background of sexually transmitted infections or due to sluggish, chronic endometritis.
Symptoms and diagnostics
The neoplasm looks like a node on a broad base or pedicle, which gradually grows from the submucosal layer towards the uterine cavity. The lesions can be single or multiple. The size of the formations varies:
-
small 0.3–0.5 centimeters;
-
average 0.6 - 1 centimeter;
-
large, more than 1 centimeter.
The growths do not have specific manifestations, which is why 10 to 24% of women with small or medium-sized nodes are not aware of the problem.

We list the most common symptoms accompanying endometrial polyp:
-
periodic pain in the lower abdomen of an aching, pulling nature;
-
excessively heavy and prolonged menstruation;
-
bleeding from the genital tract in the period between menstruation;
-
the appearance of spotting a few days before and after menstruation;
-
spotting and bleeding from the genital tract after menopause.
Most often, the formations are located in the area of the tubal angles and the fundus of the uterus, which interferes with pregnancy. And, sometimes, it is infertility that becomes a symptom that forces a woman to consult a gynecologist.
How to identify a polyp
An examination at the Universum clinic will help identify even an asymptomatic process. Non-invasive methods are used for diagnostics:
-
X-ray methods, CT;
-
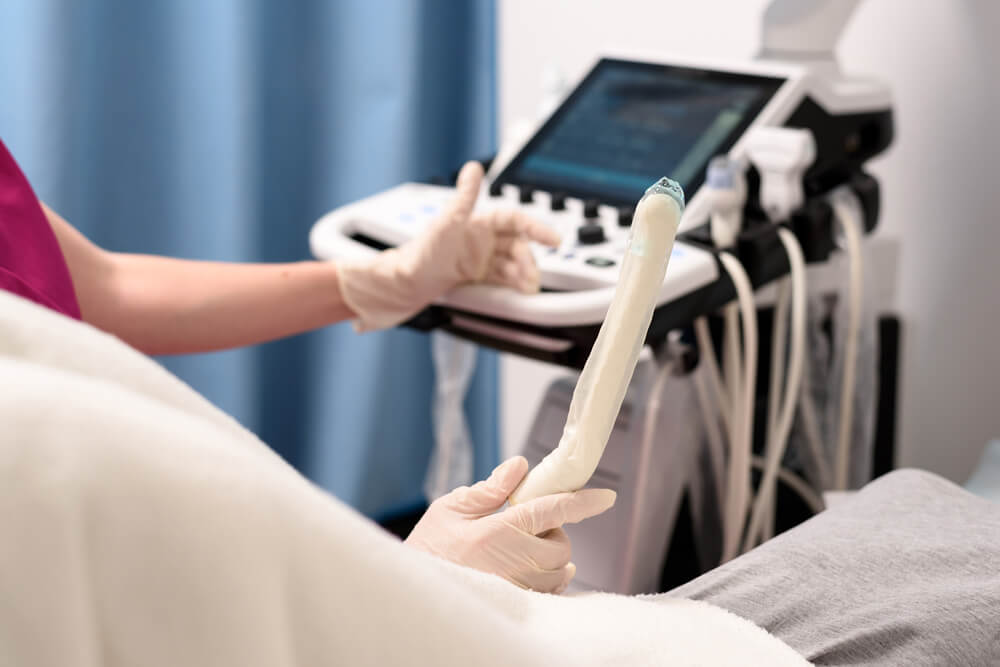
Ultrasound, including transvaginal examination of the uterine cavity with Doppler ultrasound;
-
hysteroscopy is a visual examination of the internal surface of an organ with a special endoscopic instrument.
The hysteroscope is inserted through the vagina and cervix. If necessary, the clinic’s gynecologist can take a tissue sample from the node for histological analysis to assess the nature and type of the process.
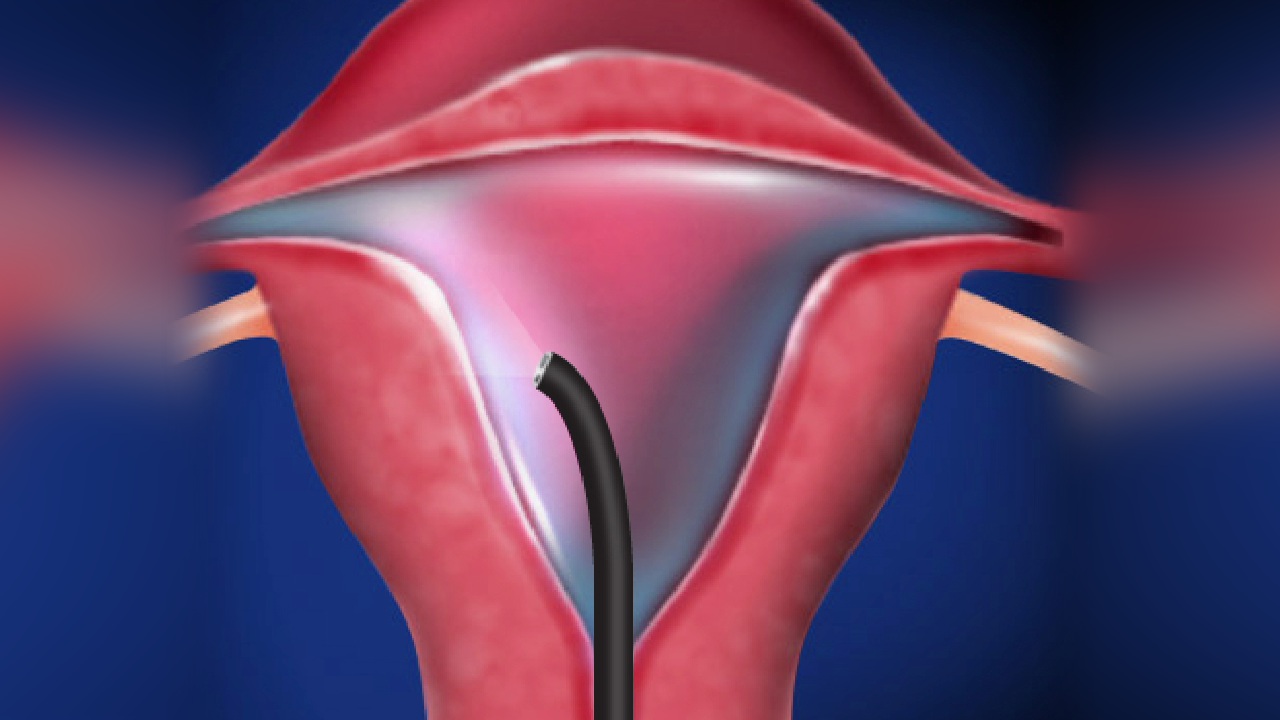
Types of endometrial polyps
Gynecologists distinguish 8 types of such pathology. Four types of neoplasms have clinical significance:
-
Glandular, with a predominance of functional cells of the uterine epithelium.
-
Glandular-fibrous, in the stroma of which appears connective, scar tissue.
-
Fibrous, the number of glandular epithelial cells in them varies from single to zero.
-
Adenomatous, with abnormal cellular composition. Such processes are dangerous due to degeneration into cancer (malignancy).
Glandular polyps of the endometrium often form in women of childbearing age with concomitant pathology. Glandular-fibrous and fibrous are characteristic of the age of menopause and after it. Dangerous adenomatous polyps are a relative rarity, but they are difficult to recognize with a hysteroscope and require a cytological examination.
What to do with endometrial polyps
The main thing is to have an appointment with an experienced gynecologist when any problems with the reproductive system appear. Or with preventive purposes, as long as there are no complaints. A Universum clinic specialist examines the patient using the most informative diagnostic techniques. Such as hysteroscopy, transvaginal ultrasound (TRUS).
The decision “of what to do” with the pathological process is made individually.
The removal of endometrial polyps is recommended for almost all women with this pathology, regardless of the size of the formation. In individual situations, intervention can be postponed unless the adenomatous variant is suspected.
First, the doctor is convinced that this is a benign process, and then chooses treatment tactics. Individually for each patient, taking into account her age and health condition, the following can be transmitted:
-
correction of the probable cause of the pathology;
-
periodic ultrasound monitoring of detected formations;
-
surgical removal of identified endometrial polyps.
In some cases, hormone therapy is indicated, but its effectiveness is considered insufficient.
To protect a woman from danger, in modern gynecology the specialists prefer to remove pathological lesions.
Methods for removing endometrial polyps
Various methods can be used to surgically treat such growths:
-
excision of endometrial polyps with a scalpel or scissors;
-
laser coagulation of the peduncles;
-
electrosurgical technique - excision of the pathological focus with a resectoscope loop.
The optimal approach is endoscopic removal of the node with its base using special instruments through the hysteroscope channel (hysteroresectoscopy).
The equipment of the LuxMedic Clinic and the qualifications of the gynecologist allow us to perform a minimally invasive procedure without complications, with a minimal risk of relapse. Both in the case of a single formation, and when there are several formations.
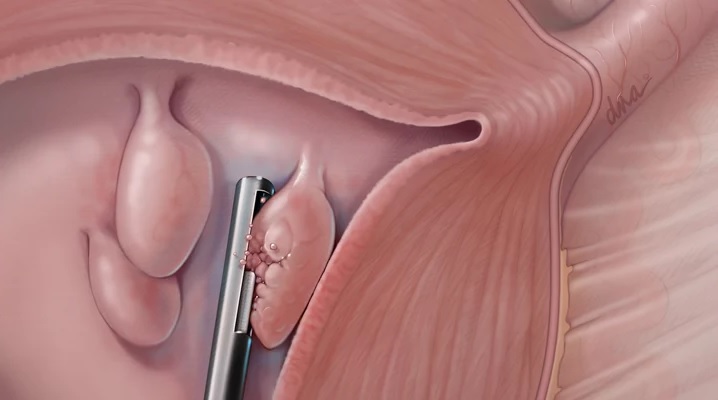
In some cases, treatment of endometrial polyps requires curettage of the uterine mucosa. Usually, this procedure should be carried out for large and multiple growths.
Contacting the LuxMedic Clinic at the first symptoms of gynecological pathology will help you avoid invasive interventions. Our specialist will conduct the examination delicately and professionally. If an endometrial polyp is detected, the doctor will select an individual, optimal treatment method.
Sources
-
Bullerdiek J, Helmke BM, Laban M. “Endometrial polyps-neoplastic lesions or not? Is it time to close the files?”, Mod Pathol. 2022 Sep 24. doi: 10.1038/s41379-022-01162-z. Epub ahead of print. PMID: 36153435.
-
Gündüz R, Ağaçayak E, Okutucu G, Alabalik U, Evsen MS. “Evaluation of definitive histopathological results of patients diagnosed with endometrial polyps: a tertiary care center experience.”, Afr Health Sci. 2022 Mar;22(1):125-132. doi: 10.4314/ahs.v22i1.16. PMID: 36032424; PMCID: PMC9382512.
-
Tong JL, Feng LM et al. [Clinical pathway for diagnosis and management of endometrial polyps]. Zhonghua Fu Chan Ke Za Zhi. 2022 Jul 25;57(7):491-495. Chinese. doi: 10.3760/cma.j.cn112141-20220422-00269. PMID: 35902782.
-
Van Gemert J, Herman MC, Beelen P, Geomini PM, Bongers MY. Endometrial polypectomy using tissue removal device or electrosurgical snare: a randomised controlled trial. Facts Views Vis Obgyn. 2022 Sep;14(3):235-243. doi: 10.52054/FVVO.14.3.035. PMID: 36206798.
F. A. Q.
-
there is a risk of degeneration into cancer;
-
the infertility can develop;
-
if growth cells synthesize hormones, the monthly cycle is disrupted;
-
there is a danger of debilitating uterine bleeding during menstruation and in the intermenstrual period.
-
If a formation is detected, it is recommended to remove it;
-
In some cases, the doctor can recommend monitoring the dynamics of the process.
-
the outgrowths enlarge, grow, and can completely fill the uterine cavity;
-
infertility develops;
-
there are risks to life due to the degeneration of the polyp into cancer, the development of anemia due to chronic blood loss.
-
the duration of the operation is determined individually, depending on the degree of damage of the uterus;
-
on the average, removal of an endometrial polyp takes from 10 to 30 minutes.







